Thank you to everyone who helped make BioDesign2025 a success.
The BioDesign 2025 Cohort
The 2025 cohort consists of six teams.
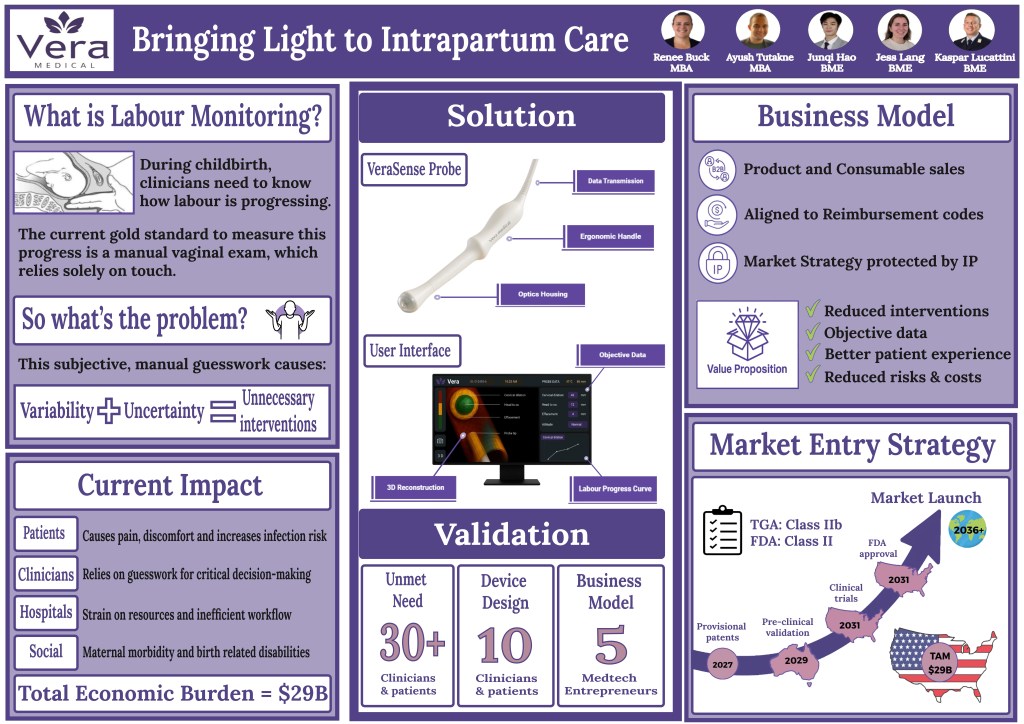
Team 1: Vera
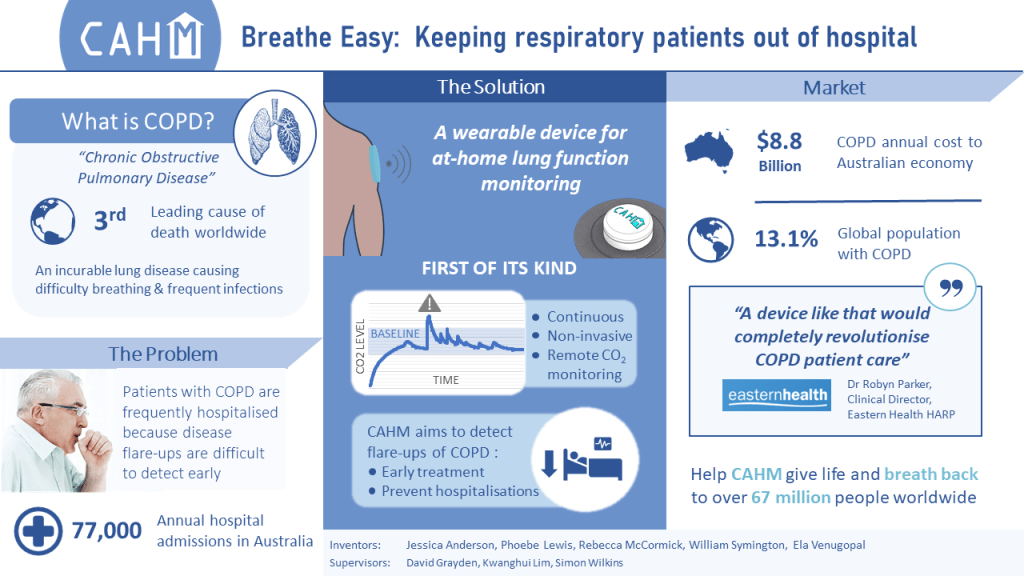
The members of Vera are Ayush Tutakne, Junqi Hao (Jackie), Jess Lang, Kaspar Lucattini, and Renee Buck. Their project is on developing a new way to detect progress during labor, helping avoid complications and improving safety leading to childbirth..
Team 2: TermWise Medical
Team TermWise consists of Anton Kogios, Gemma Melville, Steve Lau, Yeely Khoh and Winkin Kuan.
Their project is a wearable monitoring technology for preterm birth prevention. They won the prestigious $10,000 Stephen Ho award for best BioDesign project. They also won the Airwallex Award for the Endeavour project that best Enhances Social Impact Through Innovation.

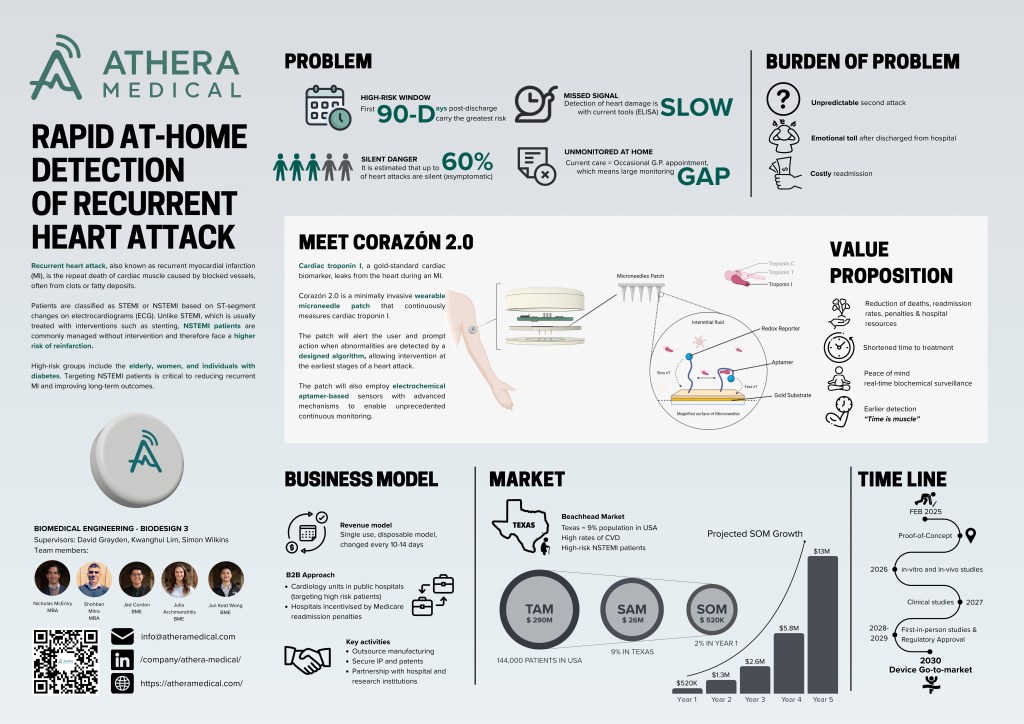
Team 3: Athera Medical
The team consists of Jad Cordon, Julia Archimandritis, Jun Keat Wong, Nicholas McEniry and Shohban Mitra.
Team Athera’s project is an at-home monitoring system post heart attack, using a new approach. Team Athera won one of two SEMBA2003 awards for best business approach ($5000).
Team 4: Encompass Medical
Team Encompass consists of Anisha Bhoyro, Dylan Cheong, Hilary McKie, Melanie Yuan and Praneel Pradhan. They are working on postpartum pelvic health to address prolapse. The team won one of two SEMBA2003 awards for best business approach ($5000).

Team 5: Dremedy
Team Dremedy is working on home tracking of immune system health for chemotherapy patients. They won this year’s prestigious University of Melbourne Research Innovation & Commercialisation Award, of which only one was awarded at Endeavour.
The team members are Aaron Toy, Adeeba Aziz, Corin Feist, David Ding, and Georgia Agati.

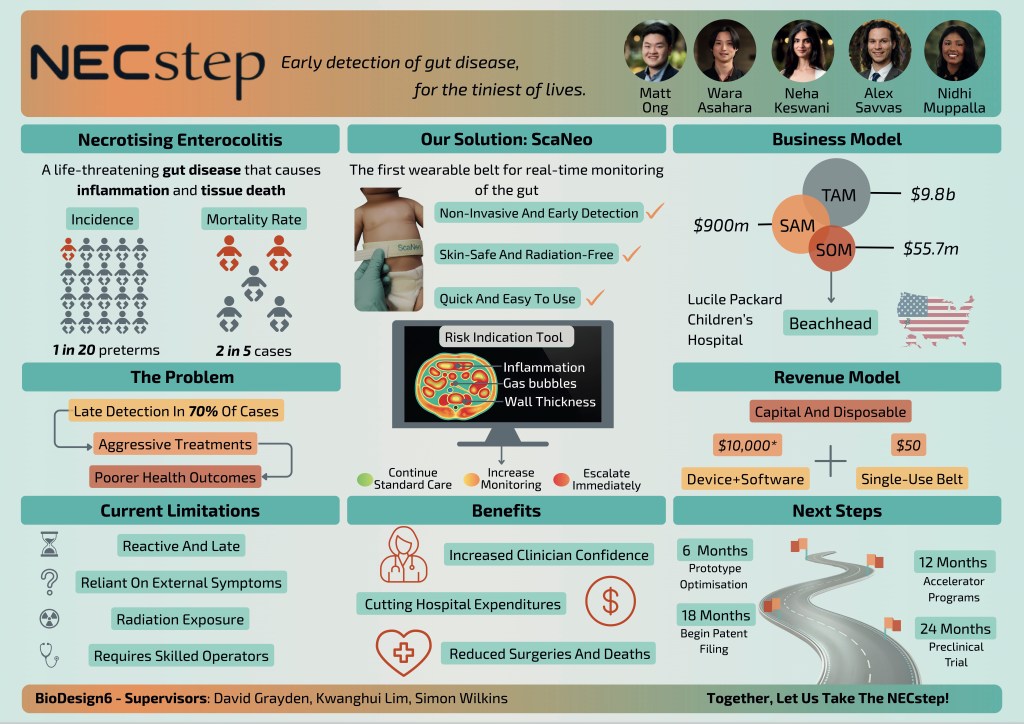
Team 6: NECstep
Team NECstep is working on early detection of gut disease in newborns, a life-threatening issue. NECstep won the $5000 Stephen Ho Award. The team members are Alex Savvas, Matt Ong, Neha Keswani, Nidhi Muppalla and Wara Asahara.