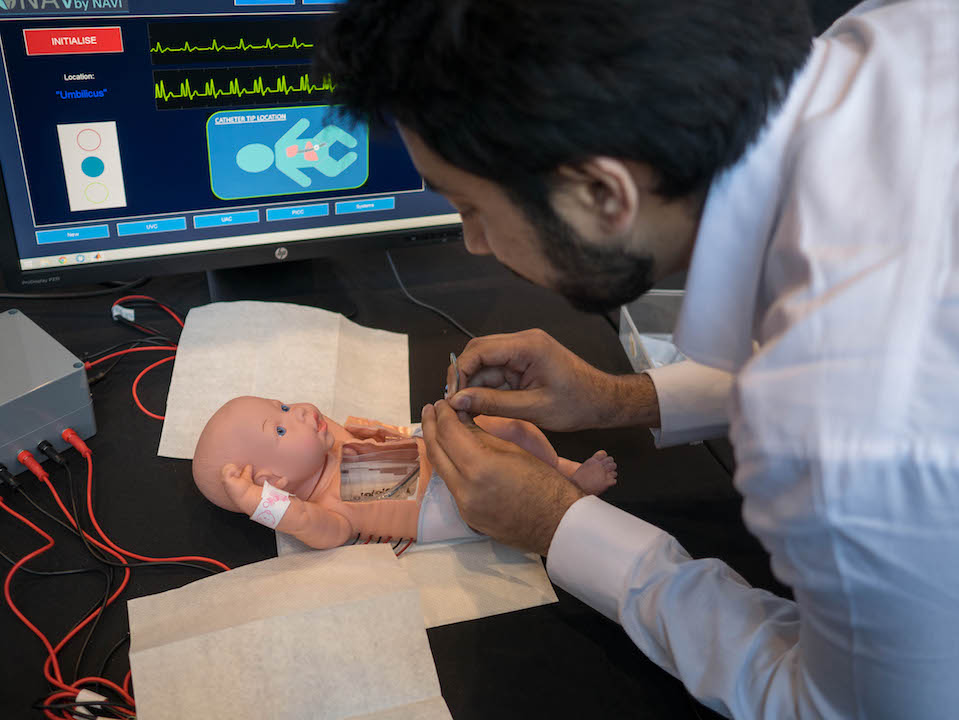
Teaching BioDesign in 2020 was particularly challenging due to Covid19. We could not have done it without the extensive help of our guest speakers, community leaders, partners organisations and colleagues.

The teaching team (David Grayden, Kwanghui Lim and Simon Wilkins) would like to express our gratitude to everyone who helped including:
Guest Speakers
- Annabella Newton, Senior Associate, Phillips Ormonde Fitzpatrick.
- Chris Farley, COO – Design @ Planet Innovation.
- David Harrison, Principal Consultant, DWH Consulting.
- Dean Freestone, Co-founder and CEO, Seer Medical.
- Denzil Furtado, Westpac Future Leaders Scholar, University of Melbourne.
- Elaine Saunders, Managing Director at Bingarra ScaleUp Solutions.
- Esther Apos, Director at CMS Scidoc.
- Guido Tresoldi, Liaison Librarian, University of Melbourne.
- Jordan Green, President and Founder, Melbourne Angels.
- Jia-Yee Lee, Associate Professor, Enterprise Fellow (Medtech), Melbourne School of Engineering at University of Melbourne.
- Kyle Slater, CPO at Seer Medical and former CEO at nura.
- Liz Williams, CEO at Hemideina.
- Leonore Ryan, Entrepreneur in Residence, TRaM Program, University of Melbourne.
- Laxmi Pun, Melbourne Accelerator Project.
- Lachlan Wilson, Patent and Trademark Attorney. Lead, Intellectual Property Team at The University of Melbourne.
- Michelle Kleynhans, Head of New Ventures, MedTech Actuator.
- Nick Opie, CTO and Founder at Synchron.
- Paul Carboon, CoFounder, Chair and CEO Microbio, Business Development @ Outerspace Design.
- Tam Nguyen, Associate Professor and Deputy Director of Research, St Vincent’s Hospital.
- Warren Rudd, Co-founder of Curvecrete.
Panelists and Special Sessions
- Prof Andrea O’Connor, Dept of Biomedical Engineering.
- Professor Dan Galai and Nadav for the special joint session with Hebrew University Jerusalem BioDesign.
- A/Prof David Ackland, Dept of Biomedical Engineering.
- Dr David Collins, Dept of Biomedical Engineering
- Professor Glenn Hoetker, MBS.
- Dr. Hamish Meffin, Dept of Biomedical Engineering.
- Associate Professor Jia-Yee Lee, Enterprise Fellow (Medtech), Melbourne School of Engineering at University of Melbourne.
- Dr. Kathryn Stok, Dept of Biomedical Engineering.
- Emeritus Professor Leon Mann, University of Melbourne.
- Prof Sandra Kentish, School of Chemical & Biomedical Engineering.
Alumni
- Alex Newton, Brad Bergmann, Mubin Yousef, Shing Yue Sheung, and Wei Sue from NAVi Medical Technologies for helping us throughout the term.
- Eric Liew, Kulaghan Kumaradevan, Edward Buijs on Needs Analysis.
- Elise Sutherland, CEO of Stelect for being a “live case” in class.
- Alumni careers panel: Wei Sue (NAVi), Wei-shen Mak (Rakutan), Ned Tyndall (CSIRO), and Sarah Fink (OMX)
Donors
- Ian Kirk whose sustained contributions to MBS makes this course viable.
- Graham Beanland and family for funding prototyping expenses and the Graham Beanland Commercialisation Award.



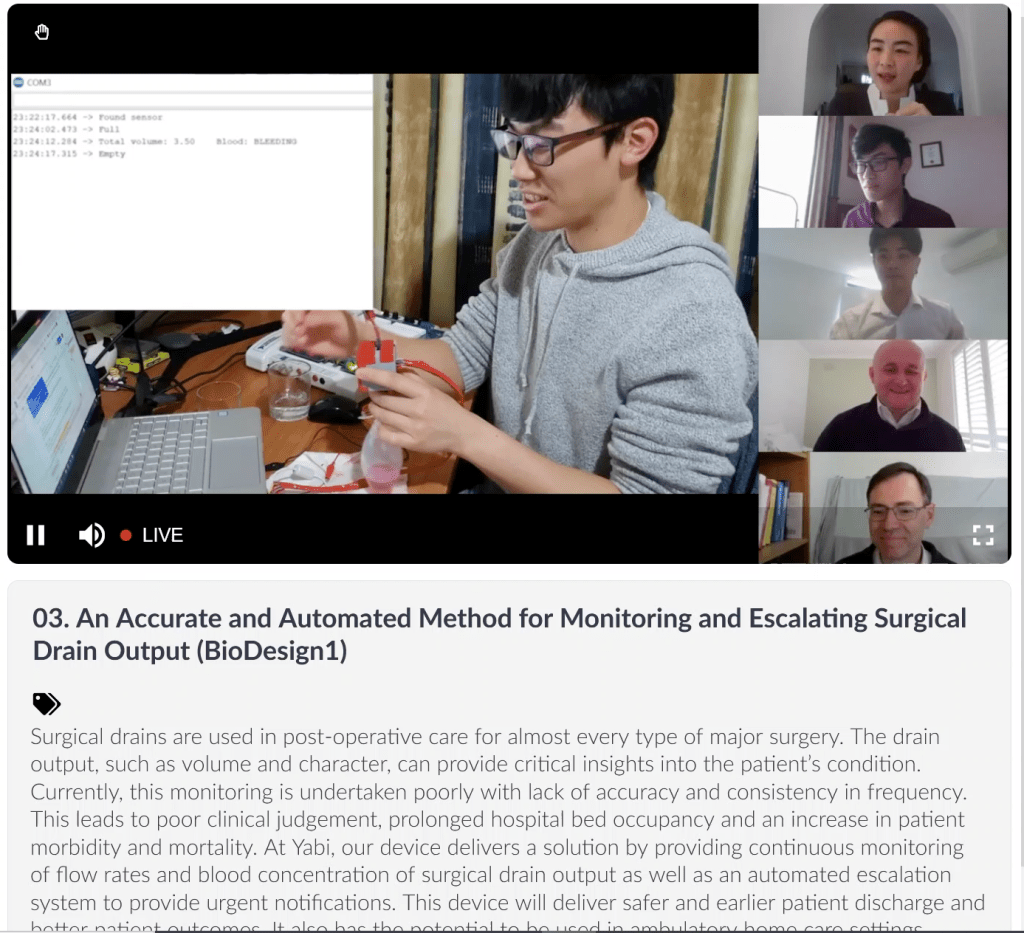

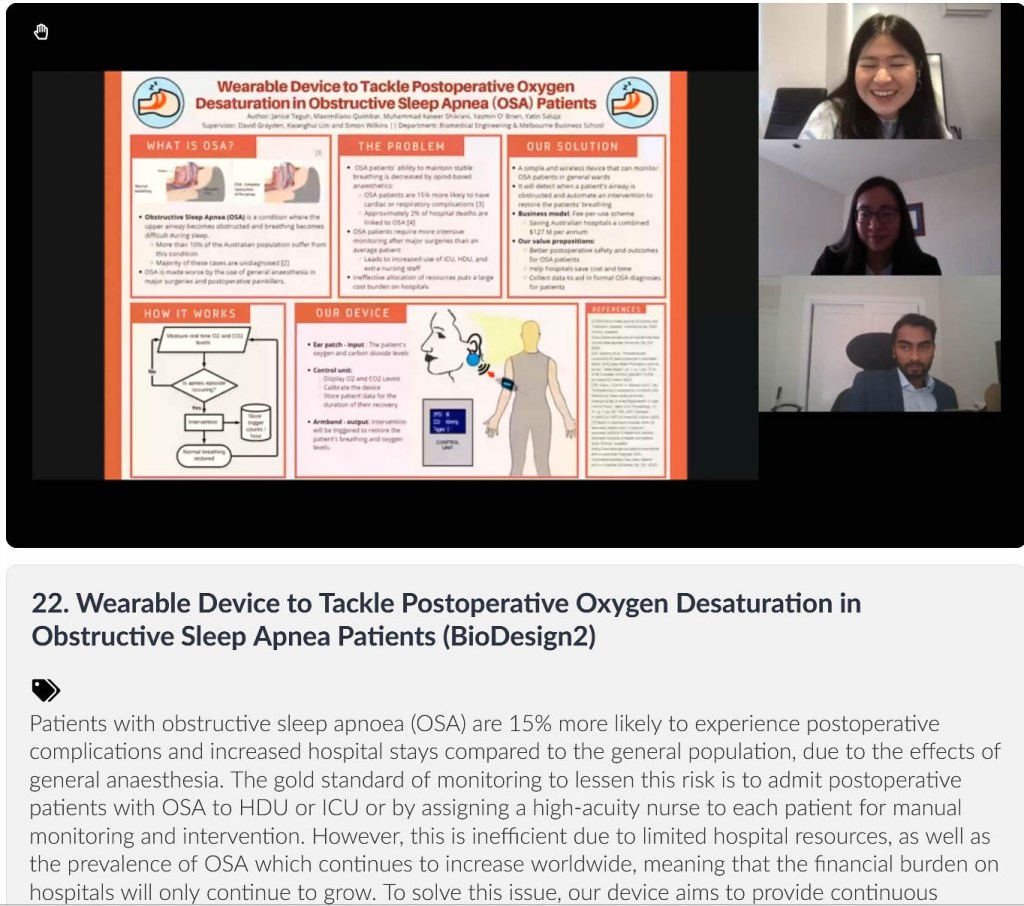

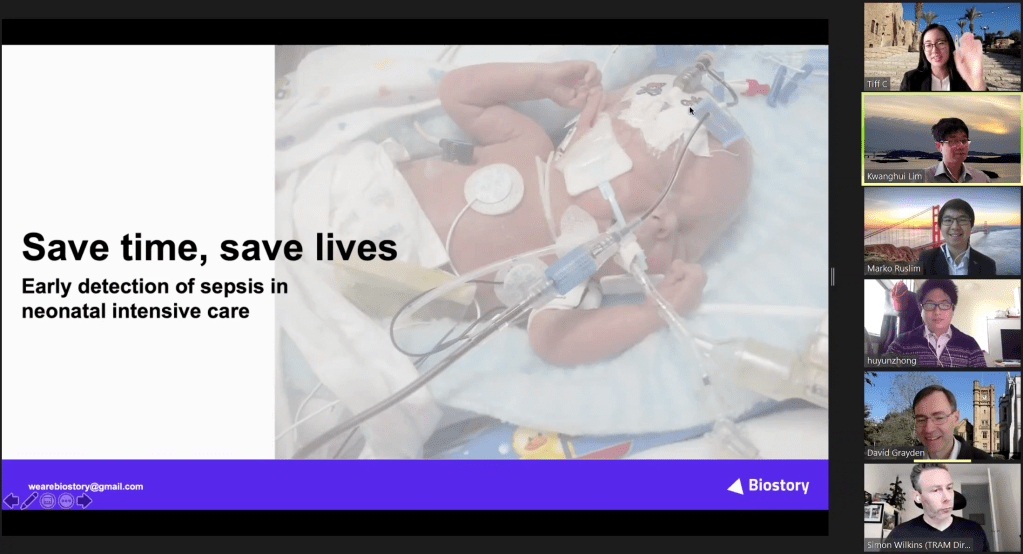
































 Team members: Hannah Merrigan, Reagan Susanto, Jason Chiang, Megan Astle, Lee Gibson.
Team members: Hannah Merrigan, Reagan Susanto, Jason Chiang, Megan Astle, Lee Gibson.